When It's Critical, It Has to Be Dwyer
Your Indoor Air Quality Solutions Provider
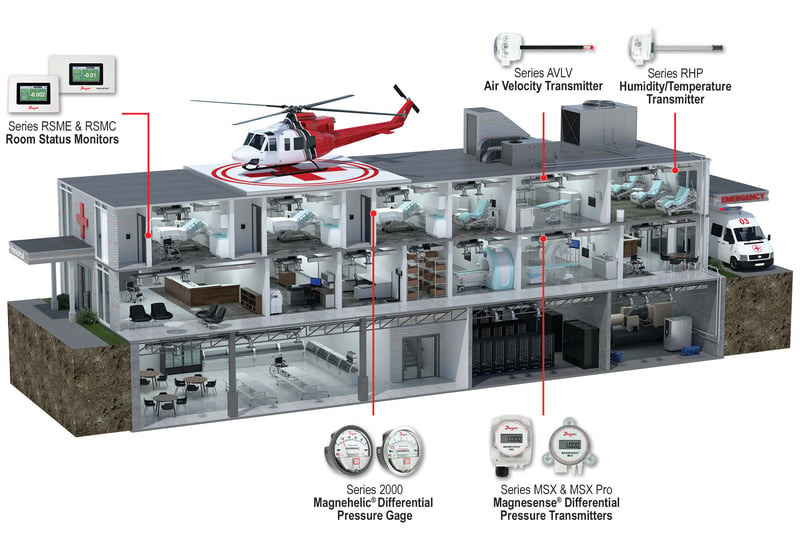
Dwyer® products are used to monitor and improve parameters that make up indoor air quality (IAQ) such as temperature, humidity, carbon dioxide (CO2), volatile organic compounds, and air changes per hour (ACH). In addition, our pressure gages are used for measuring pressure in isolation and operating rooms. Maintaining negative pressure in isolation rooms helps to keep contagions within those spaces and away from other patients or medical staff, while maintaining a positive pressure within operating rooms helps keep those areas sterile for safe medical procedures. It is vital that the indoor environment in hospitals is controlled and kept at safe levels for patients and medical staff.
Dwyer's IAQ sensors help improve environments for a safer, sustainable world.
Are you looking for one of these applications? Jump to:

Isolation & operating room pressure monitoring
A pressure differential between the room and the anteroom (a small room just outside the isolation room) is needed to prevent unwanted airborne pathogens from escaping into the adjacent rooms and hallways.
When an isolation room is kept at a negative pressure in relation to the anteroom, air from the anteroom will be pulled into the isolation room. This negative pressure relation will prevent pathogens from escaping, as no air can leave the isolation room.
Positive pressure isolation rooms and operating rooms are just the opposite. When the room is kept at a positive pressure, air from the room can be filtered out, without going back into the room. If a patient is immunocompromised or is undergoing an operation, this helps to prevent contaminants from entering the room and helps keep the patient safe.
Series RSMC StabiliSENSE™ Critical Room Status Monitor
The StabiliSENSE™ monitor features best in class long-term stability, due to its capcell technology that minimizes drift over time, resulting in less time spent calibrating and validating the performance. The 4.3” display size results in clear and accurate indications of room pressure that nurses or staff can see at a distance. Up to 4 additional sensors can be displayed on the RSMC with individual display color change indicating when other parameters are outside of room requirements such as humidity or air changes.
Series RSME Room Status Monitor
The Series RSME is a complete system with a touchscreen graphical user interface which enables access to pressure, humidity, temperature, air change, security, door status, calibration, and alarm setup. It comes standard with BACnet MS/TP and Modbus® RTU communications.
Series 2000 Magnehelic® Differential Pressure Gage
The Magnehelic® gage provides local indication of pressure difference between isolation room and corridor and allows for quick visual status of negative pressurization. Since there is no power required to function, these gages are well-suited for pop-up isolation rooms. The high accuracy option features a mirrored overlay to eliminate parallax error, ensuring a 1% accuracy.
Indoor Environmental Monitoring
Our temperature and humidity sensors are used to ensure a comfortable environment for building occupants. Beyond indoor comfort, humidity also plays a critical role in indoor air quality. Dwyer's humidity sensors can help ensure that proper humidity levels are maintained and assist in minimizing the spread of viruses/diseases and preventing mold growth.
Series RHP-E/N, RHPLC, & RHP-D Humidity/Temperature Transmitters
Dwyer’s humidity/temperature sensors feature both duct and wall mount options to fit a variety of application needs. They utilize a capacitive polymer sensing element to deliver a proportional analog output, and offer a wide selection of passive RTD or thermistor temperature sensors.
Series TE, TE-WSS, & TE-E/N Temperature Sensors
Dwyer’s temperature sensors are available in either duct, wall, or immersion mount configurations. They can be used to monitor the air or water temperature throughout a building management system or an air handler unit, or the ambient temperature in a room. Duct and immersion sensors are available with probe lengths up to 18 inches, with thermistor or RTD outputs.
Model CDSN & Series CDT, CDTR, & CDTA Transmitters
The Model CDSN or Series CDT accurately monitors the carbon dioxide concentration and temperature in indoor environments to help achieve energy savings, with digital barometric pressure adjustment for increased accuracy. The CDTR introduces additional functionality to also measure relative humidity, reducing installation time and lowering material cost. Models feature universal transmitter outputs, and various RTD or thermistor temperature sensor options. The Series CDTA combines carbon dioxide, humidity, temperature, and temperature set point with override, and features Modbus® RTU or BACnet MS/TP outputs.
Series CDTV Carbon Dioxide/Volatile Organic Compound (VOC) Transmitter
The Series CDTV senses both CO2 and volatile organic compounds (VOC), allowing it to detect fumes that may need to be exhausted in lower occupancy periods.
Series AVUL & AVLV Air Velocity Transmitters
CDC and ASHRAE guidelines state that the total volume of air in an isolation room needs to change over a minimum of 6 to 12 times per hour depending on when the hospital was constructed. Dwyer’s Series AVLV and AVUL air velocity transmitters help to meet these standards. These units provide a linear velocity output signal that can be paired with a building management system. In particular, the lower ranges of the AVLV high accuracy units are ideal for applications in quality intensive environments.

Building Energy Efficiency
Pressure sensors can be used to monitor the efficiency of the HVAC system, including the filtration of air in air handlers. When the pressure drops, it’s a sign that there is decreased air flow due to some kind of obstruction, such as particulate build-up on the filter. This will cause the HVAC system to run harder and use more energy. Knowing when to replace the filters in a system is one step to making sure that the building is as energy efficient as possible.
Dwyer also offers occupancy sensors which can improve energy efficiency by only operating lighting and HVAC systems as needed, when areas of the hospital are occupied.
Series MSX/MSX Pro Magnesense® Differential Pressure Transmitters
Dwyer’s Magnesense® differential pressure transmitters can be used to ensure proper differential pressure is maintained in the air filters installed in air handling equipment. Air filters are used to minimize the spread of particulates and pathogens and differential pressure transmitters aid in the maintenance and performance of the system by indicating the pressure drop as the filter becomes dirty.
Model OSC & OSW Occupancy Sensors
Dwyer’s occupancy sensors use infrared technology and are designed for simple installation with a wide viewing angle. Both ceiling-mounted and wall mounted units are available.

Underground Parking Garage
Furthermore, our transmitters are used in underground parking garages to monitor the carbon monoxide (CO) and nitrogen dioxide (NO2) levels emitted by vehicles. By monitoring these levels and running an exhaust fan when necessary, building owners can reduce their carbon footprint and ensure the safety of the people in the area.
Series GSTA, GSTC, CMT200, & CMS300 Gas Transmitters
Carbon monoxide (CO) and nitrogen dioxide (NO2) emissions from gasoline and diesel engines are hazardous to human health and reduce worker productivity. Managing the concentration of these fumes is essential. To minimize sensor cost and setup time, Dwyer offers combination CO/NO2 transmitters in all industry standard outputs. The Series GSTC comes with field selectable BACnet MS/TP, MODBUS® RTU, and MODBUS® communication for use with building automation systems.
Series CCS Current Switches & CCT Current Transformers
The Series CCS current switches and Series CCT current transformers are ideal for monitoring the operating status of fans, pumps, and motors. These self-powered units can be hung or tied directly to cables or wires. For use on existing installations, split core models can be installed without disconnecting cables.

Stairwell Pressurization
In modern buildings, stair pressurization systems utilize clean air from outside to push smoke (which naturally rises) back onto the floors. This helps to make sure the smoke doesn’t fill up the stairwell so occupants can breathe easier as they are making their way outside.
Running the fan continuously might waste energy and result in overpressurization (excessive positive pressure) on the fire exit door, preventing the door from opening. Therefore, the fan needs to be notified when to turn on in case of emergency.
When the fire alarm activates, a signal which starts the system is sent out, turning on the fan and differential pressure transmitter. The fan brings in fresh air from outside, while the transmitter monitors the differential pressure inside the stairwell and relays information to the damper so that it knows to remove excess air. These devices working together keep fresh air pumping into the building and the stairwell clear of smoke.
Series MSX & MSX Pro Magnesense® Differential Pressure Transmitters
The Dwyer® Series MSX Magnesense® differential pressure transmitter has the high accuracy pressure measurement required for exacting control. It uses air flow and velocity measurement to provide a linear pressure or velocity output. Additionally, this product can be used to notify both a local alarm and control system.

Air Balancing
Using an air flow hood to balance the air flow within hospitals is also important to making sure you have an appropriate number of air changes per hour. In addition, balancing with an air hood allows you to ensure rooms are properly pressurized. This helps to prevent airborne contaminants from lingering in a room or being spread throughout the hospital.
Series SAH SMART Air Hood® Balancing Instrument
The SMART Air Hood® balancing instrument, Series SAH, is easily maneuvered around obstacles like medical equipment, shelves, and cubicles. Dwyer offers skirt adapter hoods which can accommodate for the longer and larger diffusers that can be found in medical applications.
























.jpg?width=300&height=250&name=CCS%20(SPLIT%20CORE).jpg)


